REPORtES DE InVEStIgAcIón
![]()
Marian Douce.1
![]()
1 Crown College, Leadership and Culture student.
Correspondencia: Marian Douce mdouce@hcjb.org.ec
![]()
e researcher conducted this study to learn about the group of people who partici- pate in a three-year Family Practice Residency with Hospital Vozandes in Quito, Ecuador. e study investigates the residents’ basic demographics, their group iden- tity and group boundaries as well as features of their communication, educational patterns, marriage and family patterns, leadership structures and religious practices. In addition, the areas of recreational patterns, transportation practices, geographic proximity to the hospital and the residents’ influential relationship networks were studied. A relationship map, shows spheres of influence for each resident interviewed.
e strongest influencer in each participant’s life was most often their parents or spouse. Within the Hospital Vozandes’ residency program, three main influencers were identified; descriptions of each showed what characteristics they had in common.
ere also was a strong pattern of influence noted among the residents within their own year of residency.
Key words: Ethnographic Study , Family Practice, Ecuador. (Rev Med Vozandes 2011; 22(1):9-14.)
![]()
e Family Practice residents of Hospital Vozandes Quito are a diverse group of 24 people brought together by their acceptance to a three-year post graduate residency.
is study only begins to identify the rich mix of the people who go on to serve Ecua- dorians as Family Practice physicians.
e three main methods used for collecting data were: a 41-question survey (see Ap- pendix A for the survey), personal interviews (see Appendix B for the questions) and observation of the residents in four types of situations: morning report, Bible study, guest speaker presentation and university class. e researcher obtained permission from the Medical Education Department at Hospital Vozandes to present the study to the residents. Of the 24 residents in the Family Practice program, 17 signed consent forms and received a survey to fill out. e surveys were translated from Spanish to English and entered into SurveyMonkey™ to organize and analyze the results1. ere were eight core areas studied: basic demographics, group identity and group boun- daries as well as features of their communication, educational patterns, marriage and family patterns, leadership structures,2 and religious practices. ere were four elective areas studied: recreational patterns, transportation practices, geographic proximity to
the hospital and the residents’ influential relationship net- works. Special attention was given to the residents’ in- fluential relationship networks in the personal interviews.
e book Exploring the Land,3 helped to guide the rese- archer in forming questions, and in understanding and analyzing the residents’ relationship networks.
Elements Affecting the Researcher’s Bias
e researcher’s husband is the Medical Director of the hospital, leads the resident’s morning report meeting two days a week, leads a Bible study and teaches some classes to the groups of which that the residents are a part.
Before announcing the study, only some of the residents seemed to know that the researcher was the Medical Di- rector’s wife. Also, before starting the study, the researcher knew only one of the residents by name; he was in a ro- tation in a different hospital and so did not participate in the study.
e researcher’s son is a third year resident in a different program. So, although the researcher did not know the residents personally, she was predisposed to look on them favorably. She also had the bias of thinking that the Hos- pital Vozandes Quito (“HVQ”) Family Practice Resi- dency is the best one in Quito. She understands some medical terminology and her Spanish is good, but not perfect, so there is surely some bias in her choice of words translating the residents’ responses. Although the area of religious practices was not a major part of the study, the fact that the researcher is an Evangelical Missionary, and that many of the residents are not Evangelical christians lends bias in how she perceives and interacts with the re- sidents.
e researcher should have worded the survey questions 10 and 11 for group Boundary better, using “identify” instead of “define” because some of the answers gathered reflected a misunderstanding of the researcher’s intention. Question 18 “What influenced you to become a doctor?” was influenced by the researcher’s bias that having a fa- mily member, especially a parent who is a physician has great weight in a person’s choice of career. Questions 32 and 33 were influenced by the researcher’s expectation that being a resident is stressful and that recreation eases stress.
e Participants
ere are 24 Family Practice Residents total: eight first year residents, seven second year residents and nine third year residents. Of the 17 residents who filled out consent forms, 12 returned the anonymous survey forms to the teaching Department secretary.
ose surveyed included three of the eight first year resi- dents, five of the seven second year residents, and four of the nine third year residents. e researcher realizes that some of the results could have differed if all of the resi- dents had participated in the study.
Demographics
e median age of the residents filling out the survey was 28 years old with two-thirds having been residents of Quito. e others were from other Ecuadorian towns.
e majority of the respondents are single, with five being married. ose who are married have been married an average of two and a half years. It appears that most Family Practice residents marry after 25 years old. two of the out-of-town respondents live alone, and three of the married couples live just with their nuclear family.
e rest live with family or extended family and in only one case with friends. e average household income is
$1,450 per month.
group Identity
ere are 16 women and eight men in the residency pro- gram. ey regularly work 80 or more hours a week. is group identifies themselves generally with positive words both before and during the residency. ey used words such as: humane, sociable, success, happy, sincere, active, responsible, at peace, hard-working, a good person. Du- ring the residency, two also described themselves as more stressed and two as being less social than they were before the residency. is positive self and group image is reflec- ted in what the researcher observed in group interactions: animated discussions, asking bold questions, and laug- hing together even during the more sober medical lear- ning sessions.
As a group, their least confident moments were observed during Bible study. e researcher observed that although most are eager to hypothesize during medical meetings, few were willing to venture a possible “wrong” answer during Bible study discussion.
e respondents reported that doctors from other resi- dency programs generally have a positive view of the HVQ Family Practice residency: it is a good program with good teaching; the residents get along well and are respected, responsible, and holistic in their approach to patient care, serve others and are friendly and polite.
e program is also seen as demanding. Some outsiders think that these residents only treat patients who have money. Some attending physicians do not know what to
do with this new-to-Ecuador specialty of Family Practice.
group Boundaries
What sets this group of people apart from others? e re- searcher observed that this group can be identified by their clothing: all wear white lab coats with the hospital insignia and their names embroidered on the coat. All wear a hospital identification tag with their picture iden- tifying them as Family Practice residents. e men wear neckties. About half of the residents would “wear” their stethoscope around their necks.
message, written and Facebook as is shown in the follo- wing graph.
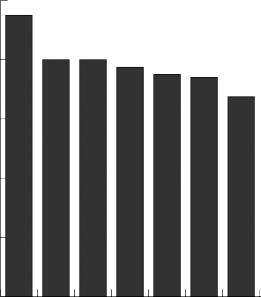
10
8
6
In the hospital setting, they can often be seen working in small groups. e researcher worded question 10 and 11 wrong on the survey, asking how others would “define” them instead of how others would “identify” them. But their answers indicated that others could identify them as residents by the type of attention they give to the pa- tients. ey are addressed as “Doctor” by those around them.
Each resident on general medicine floors works with a supervising, attending physician, an intern (last year of
4
2
0
Personal
Other 1
Phone
Text message
Written
medical school in Ecuador), and an Extern (medical stu- dent). generally, the researcher would see this group of three reporting together (minus the attending physician) during morning report.
A boundary that the researcher did not expect to find was one separating into what year of residency one was in; this was defined largely by residents identifying their best friends as other residents from their own year of resi- dency, and by a high-degree of co-operation between same-year residents. ree of the third year residents are working on their research and thesis together. e rese- archer talked with two of these three and noted a strong bond of friendship and respect within the group of three.
group communication Features
A requirement for acceptance to the Family Practice re- sidency is to read English, so it is not surprising that all of the respondents at least read English. All speak and read Spanish. Other languages some mentioned speaking and/or reading are: French, Italian, Portuguese, and Shuar. e respondent who speaks Shuar wrote that he would like to study how to do ultrasound and take this technology to the jungle.
e residents are people who really prefer personal com- munication. When surveyed about what modes of com- munication they preferred, with ten as “highly preferred” they responded that face to face is their overall preferred mode, followed by email, chat (“other 1”), phone, text
e researcher observed that much of the group learning that takes place is verbal-aural. During morning report, the doctors-in-training do not take notes. ey use men- tal pictures and mnemonic techniques for remembering complex lists. For example: “When you suspect infection, look at your hand – there are five main causes of infec- tion.” “‘ttt’ helps you remember the three causes of a chest tumor.” And “need to motivate your patients? Re- member ‘DAncRS:’ Desire, Ability, necessity, commit- ment, Responsible, Steps.”
Morning report is also a time for practicing what one would say, think and do as a doctor in a safe environ- ment: “You are the Attending. ink like a doctor! What will you ask the patient? now what tests will you order? What is the differential diagnosis? What will you tell the patient’s family?” e training that goes on during mor- ning report puts one on the spot (deliberate stress) in front of your peers. And for some this happens after being up all night.
e researcher observed that they learn, while under pres- sure, to visualize various scenarios in their heads, ask many questions, and translate complex medical terms into what to say to the patient that would make sense to the patient. Another communication tactic observed by the researcher was frequent encouragement to the doc-
tors-in-training to ask their peers for advice and help. In the researcher’s bias, she sees these people as very intelli- gent, who haven’t in the past needed to ask for help even in areas where they are stretched, and so asking one’s peers for help is a new, against-the-grain habit to develop.
Another frequent type of communication the researcher observed was confrontation. Many times during morning report, the researcher observed both the teaching physi- cian and peers challenging what the presenting doctor said. e survey asked how the resident responded to confrontation and gave several possibilities. Of the res- pondents, eight said they would give excuses or explana- tions. Other answers were: with thanks, highlight what to learn for future occasions, with patience, and with ar- guments. When the survey asked “In what way should a person confront others?” all of the responses suggested to approach confrontation tranquilly, with respect, perso- nally and objectively; that the confronter should listen patiently and then work with the other person towards improving the situation.
Educational Patterns
In Ecuador, medical school is six years long and includes college training. e sixth year is an internship year in various hospitals. e year after medical school, each gra- duate is required to do a “year of rural medicine” treating the under-served of Ecuador in various government he- alth centers.
All of the Family Practice residents have graduated from medical school with the title of Medical Doctor (“Médico cirujano”). Half of the respondents graduated from the Universidad central del Ecuador (the government’s pu- blic university in Quito), four from Pontifica Universidad catolica del Ecuador (“P.U.c.E.”), and one from Uni- versité Montpellier I. ey are all currently enrolled at
P.U.c.E. – the University that sponsors this Family Prac- tice Residency. A couple of the respondents already have other diplomas: in nutrition and Diet, and Public He- alth. Most of the respondents would like to do further studies in areas like Obstetrics, Diabetes, Ultrasound, and tropical Medicine. not surprisingly, all of the respon- dents answered “9”or “10” (out of a possible 10) to the question “For your family, how important is education?”
e most frequent reason given for becoming a doctor is the desire to help people. A second influencer was that the resident’s father was a doctor. A third reason was per- sonal desire to become a doctor.
e teaching style of the three attending physicians ob- served during morning report differed, but the objective
was the same: learn to think like a Family Practice physi- cian. e questions were fast-paced. e team of three who had been on call the previous night were expected to fully describe each patient’s status, what tests had been done, and what the possible diagnoses were. e whole group would also ask questions of the team. e team was constantly encouraged to ask for help from their peers in figuring out how to care for the patient. ey were also expected to know the wider circumstances of the patient, such as “Who is taking care of this person at home?” ey were drilled in figuring out what questions to even ask.
Marriage and Family Patterns
In general, the residents are marrying later in life than their parents did. e residents who are married, were married at an average age of 25 years old, the same as their parents. But most of the residents are still single and the average age of the single residents is 28 years old. Some residents live with parents and siblings and thus see them often. ose who are not from Quito, see family much less frequently. In interviews, it became clear that parents (especially) and siblings are a main source of in- fluence and support.
Being “on call” (working for 24 hours straight at the hos- pital) every forth night affects how often they see family. If the resident is married, the spouse usually has more in- fluence than do the resident’s parents. Four of the res- pondents have children (one child each). Family time happens more frequently in Ecuador (usually every Sun- day) than what the researcher observes happens in the United States. Also, in Ecuador, it is customary that an adult child live with his or her parents until they marry.
Leadership Structures
It is slightly more important that a resident’s bosses have leadership skills (9.4 average out of a possible 10), than that the resident has leadership skills (9.3 average). Still, out of a possible “10” in importance, this shows that le- adership skills are very important to the group.
e researcher is not aware of any formal leadership skill training happening in the residency. Leadership training might be a good addition to the residency program. In- formally, the researcher observed good leadership models and instruction. For example the residents are taught stra- tegies for motivating and helping patients, and the tea- ching physicians mentioned in interviews are sought out to give the residents their advice.
e residents preferred to have People-focused (6), En- vironmental (4) and Democratic (4) type leadership. One
preference was for Bureaucratic and two for charismatic. Please see Appendix A for the definitions of the various types of leadership from which the respondents could choose.
e key concepts mentioned in the top three preferences are: teaches his personnel (People-focused), commands by providing an ambience that inspires his followers (En- vironmental), and commands by consent, making deci- sions based on the votes of the group (Democratic).3 notably absent was the traditional “caudillo” or “strong- man” type of leadership that the researcher sees in country leaders for many Latin American countries. Why? Is this just particular to Family Practice Residents or is it indicative of a larger, generational change?
Religious Practices
Residents in the Family Practice program are chosen based on objective test results and personal interviews, though some who have good test results are in the pro- gram because of their interest in becoming medical mis- sionaries. Half of the respondents attend a church or religious institution weekly and half seldom or never do. In times of personal crisis, most would seek out advice from their parents, followed by friends, and two would ask their pastor. e Bible is the source of the respon- dent’s moral code in four cases, Baha’i scriptures for one, love for god for two others, family values influence for four respondents, and “self ” for one.
Recreational Patterns
e respondents have a wide variety of hobbies: from music and lifting weights to doing construction activities in their neighborhood to bicycling, theater, dancing and playing with their child or with their dog. Most said that since the residency started, they have very little time for recreational activities. Some do manage to fit recreational activities in nearly every day, while others might get around to their hobby once a month. Many of their stres- sors have to do with internal, personal issues: problems with so much to study, not meeting personal expecta- tions, not having sufficient personal time for family. con- flicts and unresolved problems cause stress too. Most of the stress relievers also have to do with personal issues: good communication, doing hobbies, time with family, sports, service activities, traveling, and music. Other re- creational activities are going to the mall, walking in the park, bowling, watching movies, playing with their baby, and going to the casa de la cultura museum.
transportation Practices and geographic Proximity to the Hospital
All of the respondents have traveled outside of Ecuador
to the Americas. two have traveled to Europe and Israel. travel to and from the hospital takes an average of 36 minutes one way. at means that most spend over an hour a day in travel. Half of the respondents travel by bus and half by car. e researcher’s bias and personal ex- perience in Quito would say that long travel times in crowded buses and in horrific traffic adds to the resident’s level of stress, but none mentioned daily travel as a stres- sor. Home security averages 6.7 out of 10 – “pretty se- cure.” Most of the respondents replied that home is their favorite place to relax away from the hospital.
Relationship networks
e researcher observed that the residents are friendly to each other. ey joke and laugh with each other. Most report having either the same number or more friends since starting the residency, though some commented that they don’t get to see friends from their past as often as they used to. e researcher was surprised to read that two-thirds have only one to three good friends in the hos- pital. Of the remainder, three respondents have four to six friends and one has over ten good friends in the hos- pital. So while there are good professional relationships among the residents, for most, close friendships are re- served for just a few people. close family members by far have the most influence in the residents’ lives (90%). is reflects what the researcher would expect in a culture where family relationships are close and important.
e interviews revealed more information about the re- sidents’ influential relationships. ey were asked who they see regularly, to describe some of their friends and to answer various questions about who influences them and over whom they have influence. On average, each person has seven “influencers” in their lives: three are fa- mily members (most often parents, followed by spouse); three are from the residency program, and one who is ei- ther a friend or god. e weight of that influence was shown by answers to the questions:
Whom do you ask for help in difficult times?
to whom do you tell your secrets?
Who influences the direction of your life or the deci- sions that you make?
Who is the person most listened to in your various groups?
By far, parents were mentioned most often with 20 men- tions of parents, 11 mentions of spouses and nine men- tions of people in the residency program. e family is far more influential in a resident’s life than anyone else.
ere was a pattern of the residents being more strongly influenced by residents in their same year than by resi- dents from other years. Another pattern showed up in
the interviews concerning influence within the residency program. People named six attending physicians, 10 re- sidents and one intern as people who influenced them within the program. Of those, the three people mentio- ned most by the respondents were one of the teaching physicians, the chief resident and one of the second year residents. When describing them, people used words in- dicating that each was very intelligent, good at sharing their knowledge, happy and positive, as well as helpful and available to serve others. Another characteristic that they had in common was vulnerability – asking for input from others, welcoming new ideas and being easy to get along with. One respondent commented “He never says ‘no.’ He is open to my ideas.”
e influence of the chief resident and the influential se- cond year resident was demonstrated one morning du- ring morning report. A teaching physician was reprimanding the group for not getting patient histories back into the patients’ record in a timely manner. e ambience was tense and solemn. One of the interns was stating excuses for the behavior. e second year resident and the chief resident immediately began a problem-sol- ving discussion among the 15 doctors-in-training pre- sent. Both were calm, smiling some and they helped the group come up with several ideas on how they could po- lice themselves and improve the group’s behavior. e te- aching physician was satisfied with their group-consensus plan.
e researcher enjoyed surveying the residents and pee- ring into their world. Her overall impression was that while the program is very demanding, the residents as a group are well-motivated. ey use their influential rela- tionships to help train each other to grow professionally. Most have strong support networks in their family rela- tionships and they are supportive of each other. In gene- ral, they are willing to risk guessing “wrong” answers to medical questions, but take fewer risks when the topic is spiritual in nature. Serving others is a main motivator for many in their choice of studying medicine.
From the high importance given to leadership skills, it might be helpful to the residents and their teachers to offer leadership training in future courses. It would be interesting to study how and why the characteristic of vulnerability increases the level of influence a person has on those around him or her in the residency program.
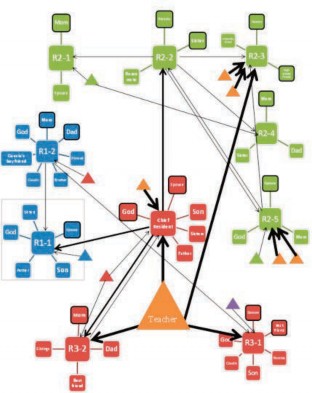
Figure 2. Above is a relationship map the researcher drew based on interviews with 10 of the residents3. The residents are marked with “R” followed by their year in residency, followed by a number assigned to the resident by the researcher. The resident’s shape is surrounded by the family and friends they identified as being in- fluential in their lives. Residents and teaching physicians who were not interviewed but who were referred to by one of the residents are marked with a triangle filled in with the color of their year. Co- lors: blue – first year resident, green – second year resident, red – third year resident, orange – teaching physician, purple – intern. Arrows showing influence go from the influencer to the person who said that person influences them. The thinnest lines are from resi- dents. The medium thickness lines are from the chief resident. And the thickest lines are from the teaching physicians. (The thicker the line, the higher in authority is the influencer.) A black line around a shape shows who the resident indicated had the most influence in his or her life.
SurveyMonkey. Available from: http://www.surveymon- key.com/
aker S. types of leadership styles [Internet]. [cited 2010 Mar 11]; Available from: http://www.scribd.com/
doc/6327744/types-of-Leadership-Styles
Bennett, S., Felder, K., & Hawthorne, S. (2009). Explo- ring the Land. Littleton: caleb Resources.